Excellence in Hepatobiliary & Pancreatic Surgery
Dr. Ding Guoping is a Chief Physician and PhD at the Department of General Surgery (Hepatobiliary and Pancreatic Surgery) of Sir Run Run Shaw Hospital, Zhejiang University School of Medicine.
Clinical Expertise
01. Biliary Calculi
Expertise in minimally invasive surgical treatment of gallstones and bile duct stones, featuring Micro-incision Laparoscopic Cholecystectomy (MILC) and tri-endoscopy combined procedures.
02. Hepatobiliary & Pancreatic Tumors
Precision treatment and minimally invasive surgery, utilizing preoperative 3D imaging assessment and advanced laparoscopic techniques.
03. Comprehensive Cancer Care
Integrated treatment for complex hepatobiliary and pancreatic malignancies, featuring full-lifecycle health management.
20+
Years Experience
600+
Minimally Invasive Cholecystectomies/Year
<20
Micro-Incision Surgery Time (Mins)
Education & Training
Chief Physician / Associate Chief Physician
Sir Run Run Shaw Hospital, Zhejiang University
Attending Physician
The Second Affiliated Hospital, Zhejiang University
Attending Physician
Ningbo No. 2 Hospital
MD / PhD in Surgery
Zhejiang University School of Medicine
Bachelor/Master of Clinical Medicine
Zhejiang University School of Medicine
Key Appointments
Committee Member
Pancreatic Diseases, Chinese Research Hospital Association
Secretary-General & Standing Committee
Biliary Tumor, Zhejiang Anti-Cancer Association
Committee Member
EBM Group, Abdominal Tumor, CMEA
Honors & Awards
Zhejiang Science and Technology Progress Award (Second Prize)
Zhejiang Province (2015)
Principal Investigator of Provincial NSF Project
Zhejiang NSF (2016)
Patient Feedback
"Dr. Ding is highly experienced and provides targeted treatment. My liver function indicators gradually decreased, and with ERCP, I recovered very quickly."
Technological Advantages
After decades of technical research, Dr. Ding Guoping has innovated the traditional laparoscopic cholecystectomy, resulting in a unique two-port micro-incision laparoscopic cholecystectomy (MILC). Compared to traditional laparoscopic cholecystectomy, it offers reduced trauma and improved cosmetic results, while demonstrating notable advantages in operational ease and applicability over single-port techniques.
| Dimension | Dr. Ding's Two-Port (Micro-incision) | Traditional Laparoscopic (3/4-port) | Single-Port Laparoscopic (SILC) |
|---|---|---|---|
| Surgical Incision | Fewer and smaller: Only two ports; the primary operating port measures just 3mm, and the secondary port is approximately 1cm. | More: Typically uses 3-4 ports; the main port is often 10mm. | Fewest: Only one incision at the umbilicus (approximately 2-2.5cm). |
| Postoperative Pain | Minimal pain: The small operating port reduces damage to abdominal muscles and nerves, resulting in very limited postoperative discomfort. | Mild pain: The additional port and larger diameter may cause slightly more pain than the two-port method. | Pain can vary: The larger single incision may lead to earlier postoperative pain, potentially even exceeding that of the two-port method. |
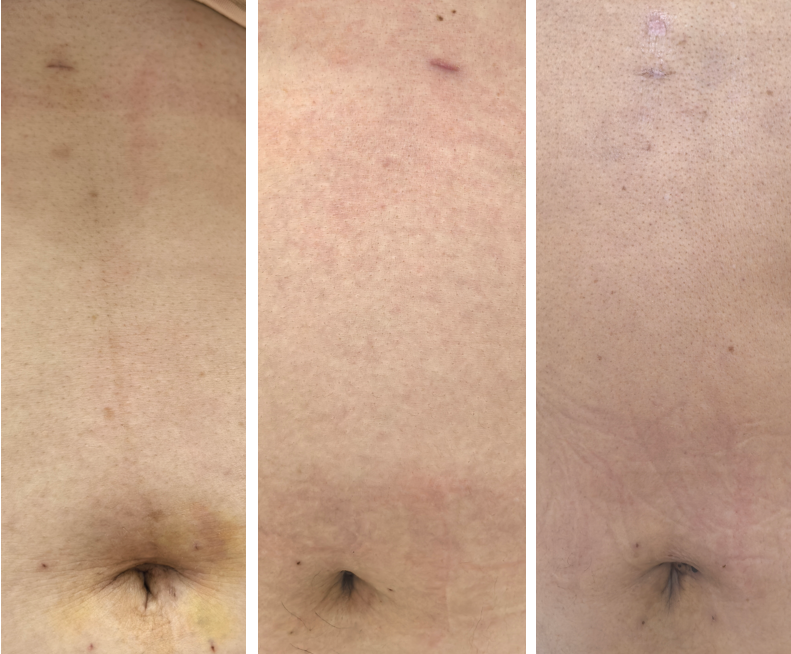
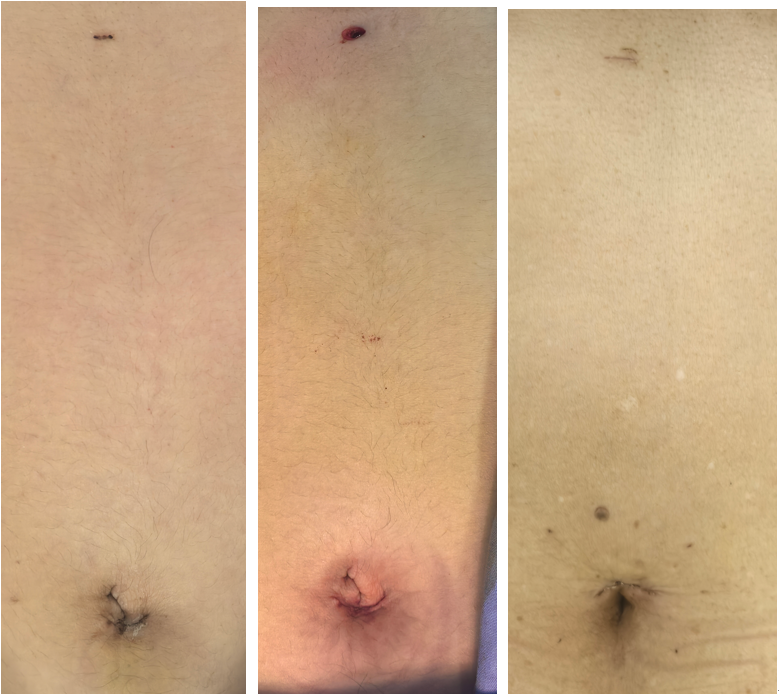
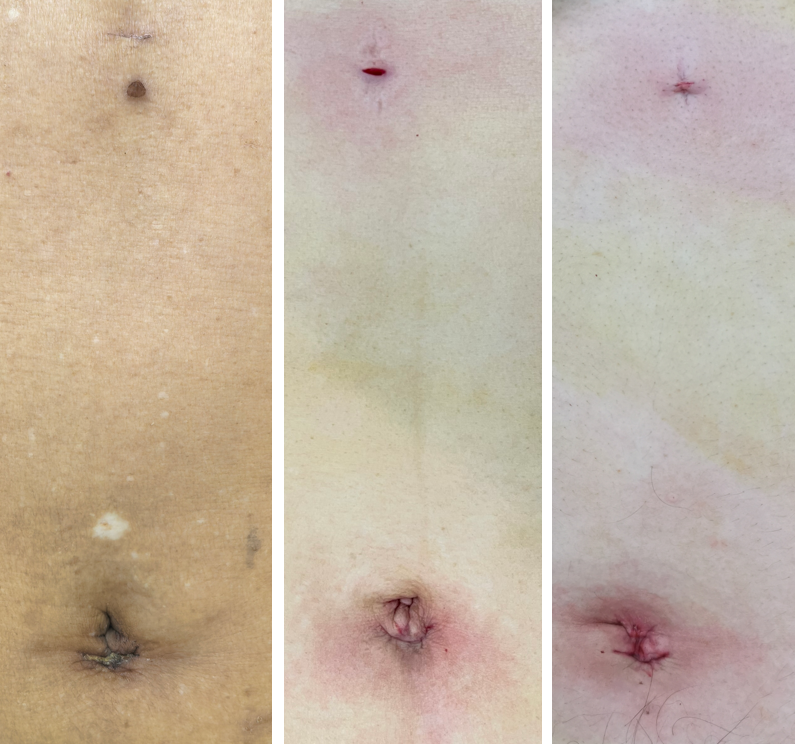
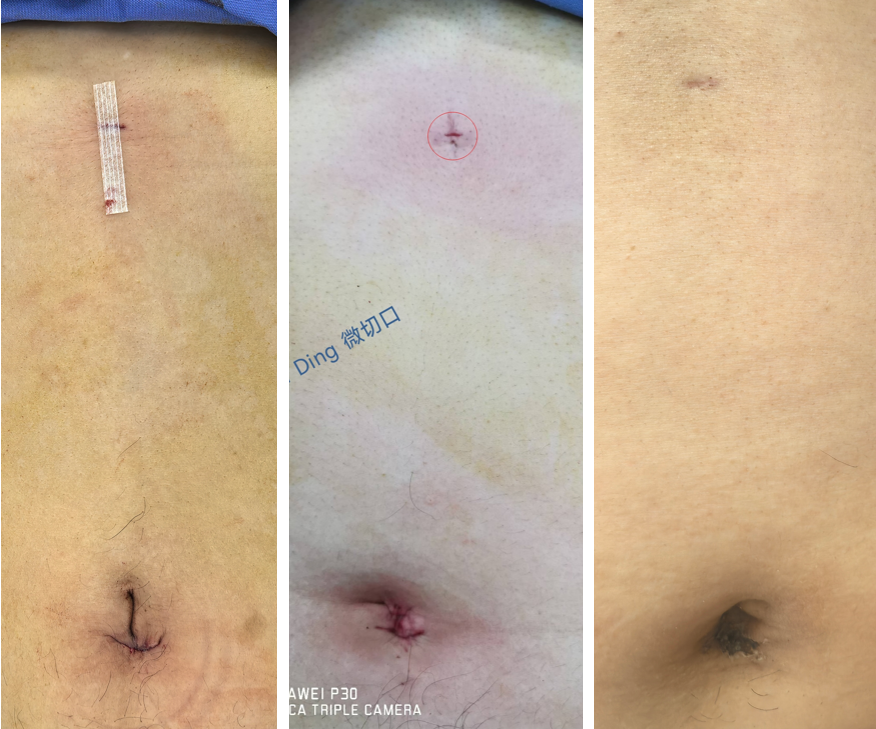
| Aesthetic Result | Barely visible scars: The 3mm primary port leaves a minuscule mark upon healing, offering excellent aesthetic outcomes. | Visible scars: Leaves multiple scattered small scars across the abdomen. | Scarless abdomen: Scars are concealed within the umbilicus. |
| Surgical Operation | Similar to traditional: Ergonomically designed with a short learning curve, minimizing instrument interference. | Ample space: Multi-angle traction is widely regarded as the 'gold standard'. | High difficulty: Instrument interference (chopstick effect) leads to a longer learning curve. |
| Surgical Time | Short duration: Typically completes in just over 10 minutes under Dr. Ding's expertise. | Medium duration: Generally takes 30-60 minutes. | Longer: High operational complexity can prolong surgery time significantly. |
| Indications Range | Somewhat limited: Suitable for most routine cases; however, traditional techniques may be employed for complex situations to ensure safety. | Wide range: Able to handle nearly all benign gallbladder conditions, including complex cases with acute inflammation. | Strictly limited: Generally only applicable for simple cases without acute inflammation or adhesions. |
Surgical Incision
Fewer and smaller: Only two ports; the primary operating port measures just 3mm, and the secondary port is approximately 1cm.
More: Typically uses 3-4 ports; the main port is often 10mm.
Fewest: Only one incision at the umbilicus (approximately 2-2.5cm).
Postoperative Pain
Minimal pain: The small operating port reduces damage to abdominal muscles and nerves, resulting in very limited postoperative discomfort.
Mild pain: The additional port and larger diameter may cause slightly more pain than the two-port method.
Pain can vary: The larger single incision may lead to earlier postoperative pain, potentially even exceeding that of the two-port method.
Aesthetic Result
Barely visible scars: The 3mm primary port leaves a minuscule mark upon healing, offering excellent aesthetic outcomes.
Visible scars: Leaves multiple scattered small scars across the abdomen.
Scarless abdomen: Scars are concealed within the umbilicus.
Surgical Operation
Similar to traditional: Ergonomically designed with a short learning curve, minimizing instrument interference.
Ample space: Multi-angle traction is widely regarded as the 'gold standard'.
High difficulty: Instrument interference (chopstick effect) leads to a longer learning curve.
Surgical Time
Short duration: Typically completes in just over 10 minutes under Dr. Ding's expertise.
Medium duration: Generally takes 30-60 minutes.
Longer: High operational complexity can prolong surgery time significantly.
Indications Range
Somewhat limited: Suitable for most routine cases; however, traditional techniques may be employed for complex situations to ensure safety.
Wide range: Able to handle nearly all benign gallbladder conditions, including complex cases with acute inflammation.
Strictly limited: Generally only applicable for simple cases without acute inflammation or adhesions.
Clinical Cases
Pioneered Micro-incision Laparoscopic Cholecystectomy (MILC)